Prostate Cancer Screening
 It will come as no surprise to many that one of the most common conditions that men ask about screening for is prostate cancer.
It will come as no surprise to many that one of the most common conditions that men ask about screening for is prostate cancer.
Prostate cancer is relatively common and is increasingly likely to affect men as they get older, rising from almost none at age 45 to 8 new cases identified per thousand men at age 70. It is not much of an exaggeration to say that every man who lives long enough will get prostate cancer.
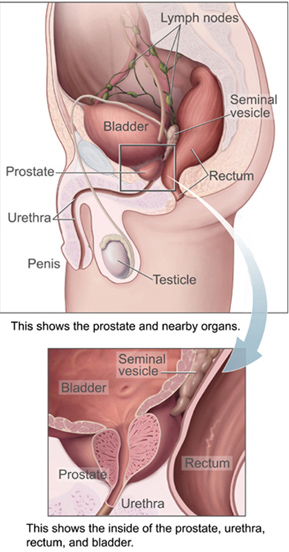
Fortunately, because the prostate gland is wrapped around the urethra (the tube that takes urine from the bladder to the outside) prostate cancer often causes early symptoms which men can detect.
Although these symptoms also indicate harmless disease, we advise ALL men with ANY of these symptoms to speak to a doctor quickly.
- Hesitancy - taking a little longer than usual to start passing urine.
- Poor Stream - the flow of urine is not as strong as it once was.
- Dribbling - persistent dribbles after the main flow of urine has ended.
- Nocturia (Getting up at night to pass urine) - getting up at night has many causes - if prostate related, usually there are other symptoms too.
- Blood in the urine or semen - this is not just for prostate cancer. Blood in the urine is NEVER normal and ALWAYS needs investigation.
For men who have these symptoms, a rectal examination and a PSA (prostate specific antigen) blood test are useful to assist in ruling out prostate cancer.
The difficulty arises when we try to use PSA to screen men who have no symptoms but who would like to have the condition excluded.
Sadly, the test cannot tell for certain whether a cancer is present or not. Neither can it tell whether any cancer detected is aggressive and likely to require treatment, or relatively harmless and unlikely to cause a problem. In order to improve the test, research has been undertaken which has identified the PSA levels in many men of all ages who have prostate cancer and we set our upper limit of normal according to age, with the intention of detecting 95% of all men with prostate cancer. Unfortunately, 10-15% (or about 1 in 8 to 10) of men who do not have prostate cancer will also have PSA levels above this nominal upper level of normal.
The difficulty mentioned above occurs because there is a reasonably wide range of PSA test results found in both healthy men and those affected by prostate cancer. There is a substantial overlap between the test results of healthy men who happen to have a slightly higher than average PSA and men with cancer who have no significant rise in their PSA levels. This issue is not unique to PSA - it is a problem with many tests for many conditions.
If you are confused after reading this, YOU ARE NOT ALONE! Please discuss this with your doctor.
The PSA Dilemma
In order to understand whether PSA screening is useful or not, it is most helpful to discuss an example and when examples are used it is only right that we should explain why we chose the example we did. In this case, we illustrate a sample of men who are in the age group most likely to ask about PSA screening. For the age goup 55 to 64, US statistics for white and hispanic males (who have similar risks) suggest that close to 1 in 200 men will have prostate cancer. NOTE: the risk for men of African origin is MUCH higher and these statistics do not apply to this one racial group.
Consider therefore, 200 men without symptoms who choose to undergo PSA testing
30 men will have positive tests. (one eighth of 200)
All 30 will have to undergo further investigation including ultrasound testing, further blood testing and possibly prostate biopsy. Prostate biopsy has an 85% rate of significant complications (mainly pain and bleeding of short duration) but is associated with severe infection in a few cases and also, rarely, death. Even a prostate biopsy can miss prostate cancer (about 10%) and so the tests may have to be repeated after a while, just to be on the safe side.
1 man has prostate cancer. The PSA test has a 1 in 20 chance of missing this man and giving him a 'normal' result. There is no way to be sure that this man is included in the 30 with positive tests.
Because of the low risk of prostate cancer (1 in 200) in men aged 55 to 64 and the fact that you are 30 times more likely to have a positive test than you are to have prostate cancer, we DO NOT recommend routine PSA testing for men with no symptoms of prostate cancer.
That having been said... There have been two recent trials looking into whether PSA screening has survival benefits. Neither trial showed significant population level survival benefits from prostate cancer screening using PSA. It is possible to reduce prostate cancer specific mortality (the amount of deaths related to prostate cancer directly) by screening but not to improve overall life expectancy. If you take the most optimistic view of screening, then screening 1000 men for 10 years will prevent one death from prostate cancer.
So why does screening for prostate cancer not help improve survival?
This is due to the nature of the cancer and the complications of treatment.
It stands to reason that during the development of any cancer, there is a single moment in time before which it was confined to the original tissue, in this case the prostate gland, and after which it has spread elsewhere. Before that moment, removing the cancer is life-saving, afterwards it may be unhelpful or even harmful.
We are unable to detect very small amounts of tumour that may already have spread so when you have an organ removed for cancer you have to hope that it was removed before spread has occurred - unless the spread is obvious, there is no way to be sure.
Thus, when you have a positive PSA test AND cancer is found on biopsy is it impossible to be sure whether your cancer has spread (and aggressive treatment is unhelpful) or not (in which case it may save your life)
This is further complicated by the fact that it is impossible to be certain whether a prostate cancer is going to follow an indolent course and do you no harm or a fulminant one and kill you quickly. We can give a probability but almost all cancers that have no uncertainty about their aggressive nature have already spread when detected. Remember that most prostate cancers are unlikely to kill.
Given that most prostate cancers that are likely to be lethal spread rapidly, there is little chance of detecting one before it spreads, so most prostate cancers that are detected are either never going to spread or have already done so.
Further, the treatments for prostate cancer are not harmless and carry significant risks of harm, meaning that patients are almost as likely to be killed by the complications of treatment as they are to have their lives saved by it.
Wider availability of prostate MRI scanning is likely to reduce the risk of overtreatment and overdiagnosis, though in New Zealand at least, access to this is still quite limited (as of Oct 2020). If we can improve scanning technology further then the risk:benefit ratio will over time move into screening being more worthwhile.
Further discussion may be found here: http://www.cancer.gov/cancertopics/factsheet/detection/PSA
So why do some doctors recommend PSA screening?
It may seem strange, but doctors have a positive incentive to recommend PSA testing. Seen from the point of view of a doctor, it is a no-lose scenario.
If you have a normal PSA, you are happy and even if you do have prostate cancer, your doctor did his best.
If you have an abnormal PSA, you are grateful to your doctor for arranging the test and any complications are seen as the inevitable result of important tests, not the fault of the doctor.
The only way a doctor can lose is by not recommending the test, even though the evidence at present suggests he should not and you are far more likely to be harmed by it than to have your life saved by it.
Yes, doctors should be more robust than this, but not all are. There is still debate over how the two major PSA trials should be interpreted, though the majority of authorities have recommended against PSA screening based on their results. There is also a lot of effort from well-intended charities who use high-profile celebrities to push the case for PSA testing, against the weight of evidence and this leads to patients being very keen on PSA testing.
It remains your choice.
The purpose of this article is to inform you, not to persuade you or tell you what to do. Though by dint of the weight of evidence, the conclusion has to be that PSA testing is unhelpful in general, whether the harms of an investigation or treatment outweigh the benefits has to be an individual choice.
Remember that any investigation is a matter for discussion between you and your doctor and that testing is the right thing for some people and not others.
We are very happy to consider requests for PSA testing, especially when patients have been informed by reading articles such as this one.
If you do decide to have a screening test, we recommend that they are done at an interval determined by your most recent test result. In studies, men with a result less than 1ng/ml developed no prostate cancer over 5 years. If your result is less than 1, you could consider re-testing in 5 years. A result of 2 or less would require re-test in 2 years and over 2 in 1 year.
Prostate or Prostrate?
The correct spelling is the former - PROSTATE with no second R. Prostrate means to lie down with your face towards the floor, often in an act of supplication or devotion. The two are very different, despite the common mis-use of the word prostrate in the media!
Further Reading
Whilst this is not intended to be a reference work, it may be helpful to read some of the research that has helped to inform this article.
Overdiagnosis and overtreatment of early detected prostate cancer this is a full article available to view free. It is well-founded and discusses the current situation in the context of the consideration of prostate cancer being overdiagnosed without clear benefit. A key quote, itself from the abstract of another paper is "approximately 73 patients will require radical treatment for each prostate cancer death averted. This translates into a 3- to 4-week survival benefit, unadjusted for quality of life" The original abstract can be found here. It is important to note that this includes a thought model potentially treating ALL cancers with radical prostatectomy, rather than as is current practice, selecting some for observation. It does NOT say that you only have a 1 chance in 73 of gaining minimal benefit from prostatectomy.
Last updated 16/20/2020, 06/05/2019